Sandata Billing Reports

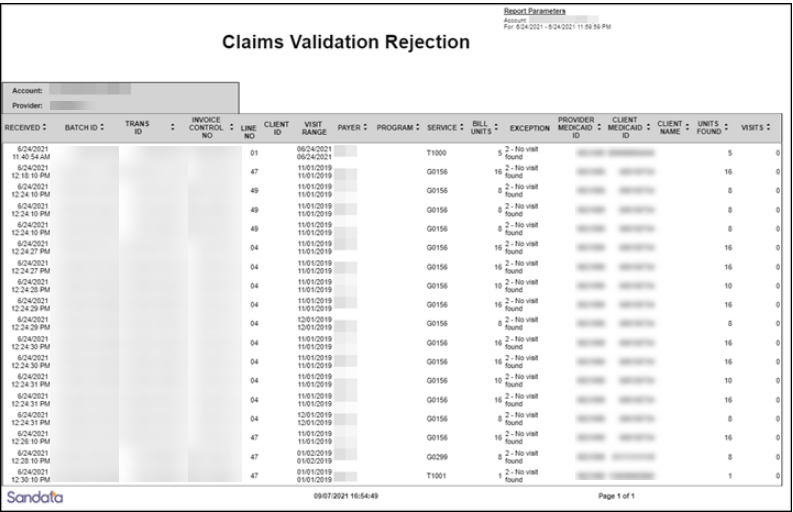
This report shows all claims validation requests that were returned unsuccessfully by the Sandata’s Claims Validation system. The report shows the request including the error message returned.
Use this report to quickly identify claims where matching EVV information was not found. This can assist in identifying visits that require action so they can be resubmitted to the claims validation system.
Use the following fields to limit the report output:
| Field | Description |
|---|---|
| Payer | visits for the selected payer(s) |
| Program | visits for the selected program(s) |
| Service | visits for the selected service(s) |
Reports are grouped by the following fields. Each change in these fields results in a page break.
| Field | Description |
|---|---|
| Account | the provider agency’s Sandata EVV account number |
| Provider | the state assigned identifier for the prover (e.g Provider Medicaid ID) |
Each column of the report lists:
| Columns | Description |
|---|---|
| Received | the date the claim was received by Sandata Claims Validation |
| Batch ID | the batch ID number for the claims validation request |
| Trans ID | the transaction ID number for the claims validation request |
| Invoice Control NO | the invoice control number for the claims validation request |
| Line NO | the line number within the invoice |
| Client ID | the Sandata client ID |
| Visit Range | the date range for the claim where the visits were reviewed |
| Payer | the payer for the claim line |
| Program | the program for the claim line |
| Service | the service for the claim line |
| Bill Unit | the billable units for the claim line. This reflects the total billing requested for the date range |
| Exception | the information returned for the failed claims request |
| Provider Medicaid ID |
the client's Medicaid ID and/or Alternate Medicaid ID If not available, Payer ID. If newborn support is enabled and the client is flagged as a newborn, this field shows an N. |
| Client Name |
the client's name. Blank if unknown. |
| Units Found | the total billable units for all visits found matching the request criteria |
| Visits | the number of visits found which were reviewed for the claims request |
Sample Report

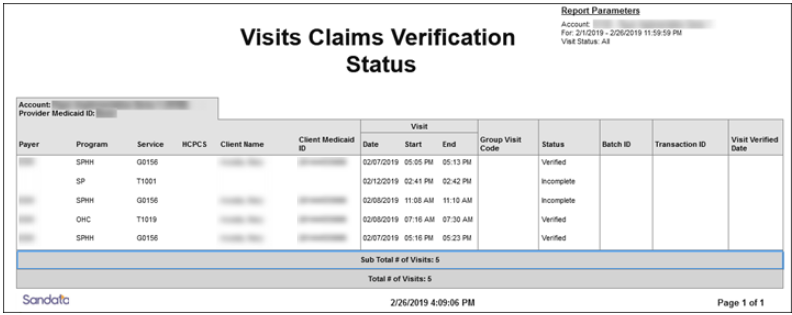
This report displays all visits within the selected date range and shows the last time each visit was returned to the payer for validation.
Use this report to track the status of visits relative to claims validation. It can be used to review when a particular visit was returned to the adjudicating system.
Use the following fields to limit the report output:
| Field | Description |
|---|---|
| Payer | visits for the selected payer(s) |
| Program | visits for the selected program(s) |
| Service | visits for the selected service(s) |
| Client Medicaid ID | visits for the client's Medicaid ID |
| Supervisor | visits for the selected supervisor at the provider agency |
| Visit Status | visits for the selected visit status |
Reports are grouped by the following fields. Each change in these fields results in a page break.
| Field | Description |
|---|---|
| Account: | the selected provider |
| Provider Medicaid ID: | the provider's Medicaid ID and/or Alternate Medicaid ID |
Each column of the report displays:
| Columns | Description |
|---|---|
| Payer | the payer for the related visit |
| Program | the program(s) fir the visit |
| Service | the service performed for the visit |
| HCPCS | the HCPCS code used for billing |
| Client Name |
the client name Blank if unknown |
| Medicaid ID |
the client’s Medicaid ID and/or Alternate Medicaid ID If not available, Payer ID. If newborn support is enabled and the client is flagged as a newborn, is shown as “N”. |
| Visit Date/Start/End | the date, start time and end time of the visit |
| Group Visit Code | the group visit code associated with the visit, if applicable |
| Status | the status of the visit |
| Batch ID | Currently Unavailable |
| Transaction ID | Currently Unavailable |
| Visit Verified Date | Currently Unavailable |
Sample Report